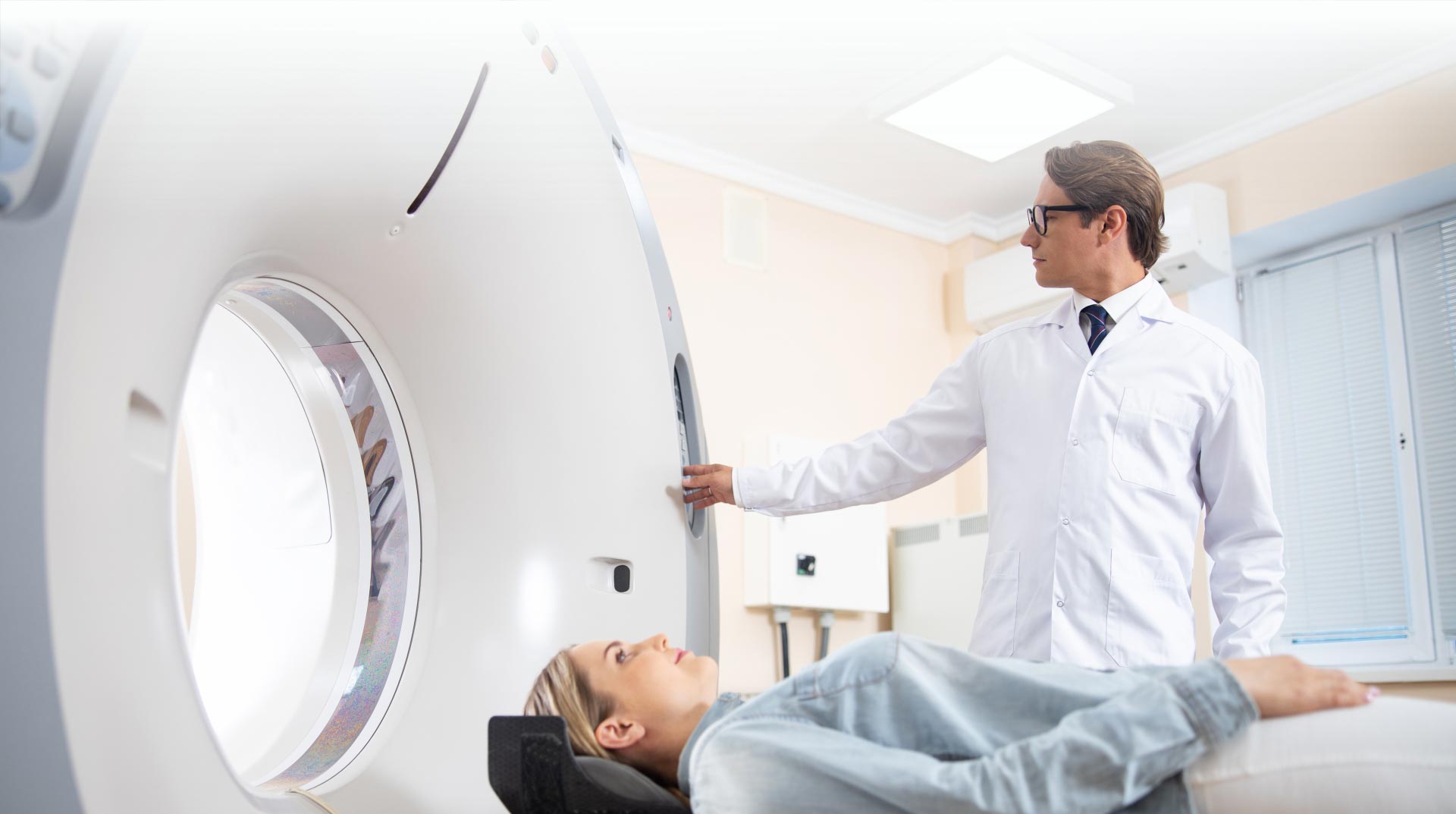
MRI
CT SCAN
X-Ray
Dexa
Ultrasound
Echocardiogram
Welcome to Advanced Magnetic Imaging Center Located in West New York, NJ
At Advanced Magnetic Imaging, we offer a wide range of diagnostic services including MRI, cat-scan, vascular ultrasound, general ultrasound, X-ray, bone density, echocardiogram, and much more. For more information, contact us, or request an appointment online. We serve patients from West New York NJ, North Bergen NJ, Union City NJ, Guttenberg NJ, Weehawken NJ, Hoboken NJ, Fort Lee NJ, Englewood NJ, East Rutherford NJ, Jersey City NJ, and the surrounding areas!
Welcome to Advanced Magnetic Imaging Located in West New York, NJ
At Advanced Magnetic Imaging, we offer a wide range of diagnostic services including MRI, cat-scan, vascular ultrasound, general ultrasound, X-ray, bone density, echocardiogram, and much more. For more information, contact us, or request an appointment online. We serve patients from West New York NJ, North Bergen NJ, Union City NJ, Guttenberg NJ, Weehawken NJ, Hoboken NJ, Fort Lee NJ, Englewood NJ, East Rutherford NJ, Jersey City NJ, and the surrounding areas!


Vascular Ultrasound
Vascular ultrasounds play a critical role in the diagnosis of a wide range of vascular diseases affecting the blood vessels. Vascular diseases can be serious and lead to a number of adverse health outcomes in the absence of early detection and treatment intervention.

Vascular Ultrasound
Vascular ultrasounds play a critical role in the diagnosis of a wide range of vascular diseases affecting the blood vessels. Vascular diseases can be serious and lead to a number of adverse health outcomes in the absence of early detection and treatment intervention.


CHECK OUR BLOGS
KEEP UP TO DATE WITH THE NEWS BLOGS

APPOINTMENT REQUEST
WE WILL CALL YOU TO CONFIRM YOUR APPOINTMENT
CHECK OUR OFFERS
TAKE ADVANTAGE TODAY
CHECK OUR BLOGS
KEEP UP TO DATE WITH THE NEWS BLOGS

APPOINTMENT REQUEST
WE WILL CALL YOU TO CONFIRM YOUR APPOINTMENT
CHECK OUR OFFERS
TAKE ADVANTAGE TODAY